AppId is over the quota AppId is over the quota Editor’s Choice
Academic Journal
Main Category: Nutrition / Diet
Also Included In: Eczema / Psoriasis;??Respiratory / Asthma;??Pediatrics / Children’s Health
Article Date: 15 Jan 2013 – 0:00 PDT Current ratings for:
Fast Food Linked To Asthma And Eczema In Kids


Kids who eat fast food three or more times a week are likely to have more severe allergic asthma, rhinitis (hay fever), and eczema.
The finding came from new international research and was published in the journal Thorax.
Similarly, a previous study demonstrated that the benefits of breastfeeding in preventing asthma are cancelled out by eating fast food once or twice a week.
The results of the new study motivated the investigators to believe that a fast food diet may be playing a part in the increase in these conditions. If a causal relationship is found, it could have major importance to public health, considering how popular these fast food places are.
Over 319,000 thirteen to fourteen year olds from 51 countries and over 181,000 six to seven year olds from 31 countries were involved in the study. All of the subjects were enrolled in the International Study of Asthma and Allergies in Childhood (ISAAC), the largest of its kind involving over 100 countries and almost 2 million kids.
The teenagers and the parents of the kids were asked questions regarding symptoms of asthma (wheeze), eczema, rhinoconjunctivitis (runny or blocked nose along with itchy, watery eyes), and their diet on a weekly basis.
The severity of the symptoms that occurred over the past year were assessed through the questions, including how frequent they were and whether or not they interfered with daily routines or sleep patterns.http://www.eczemablog.net/
/ABS/Auto%20Blog%20Samurai/data/Eczema%20Blog/e/256px-Fast_food_%2528282678968%2529.jpg)
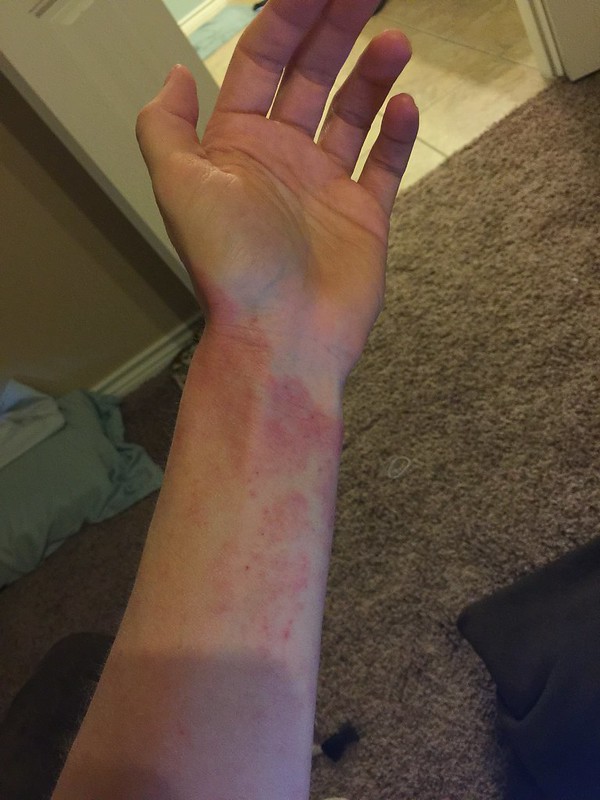
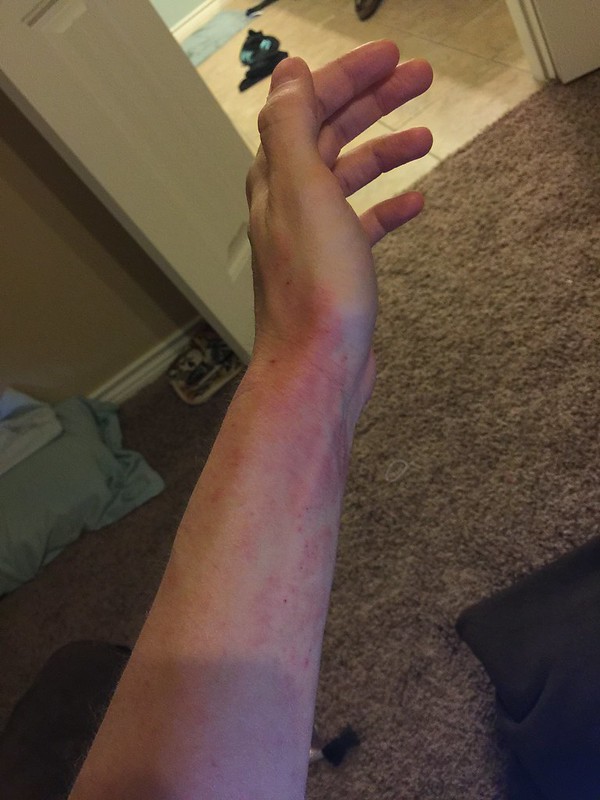
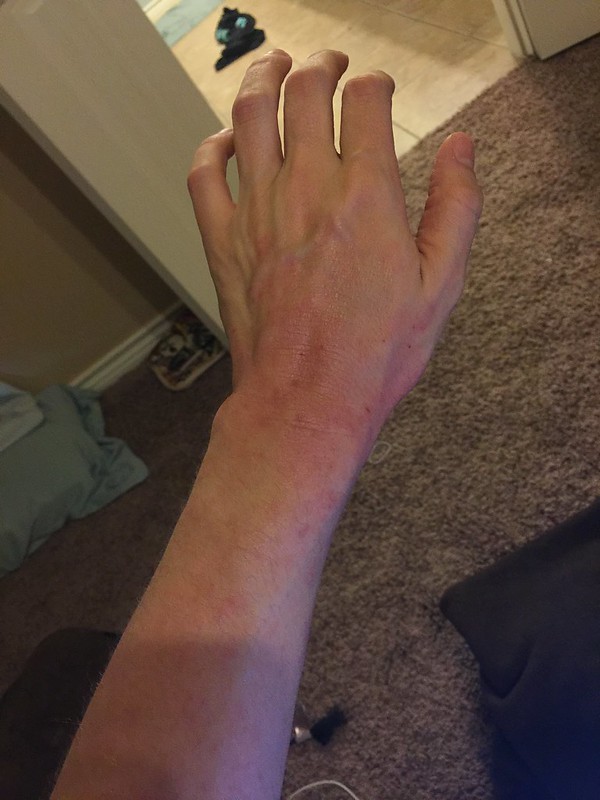
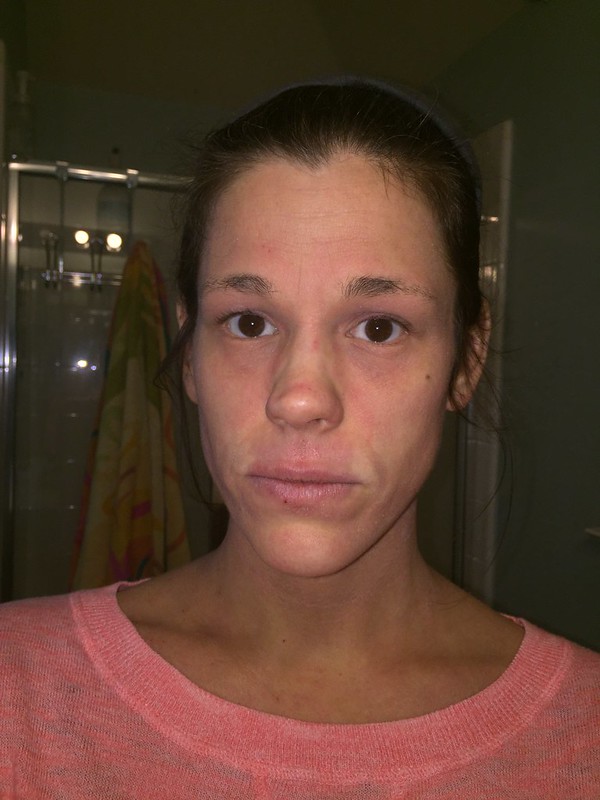
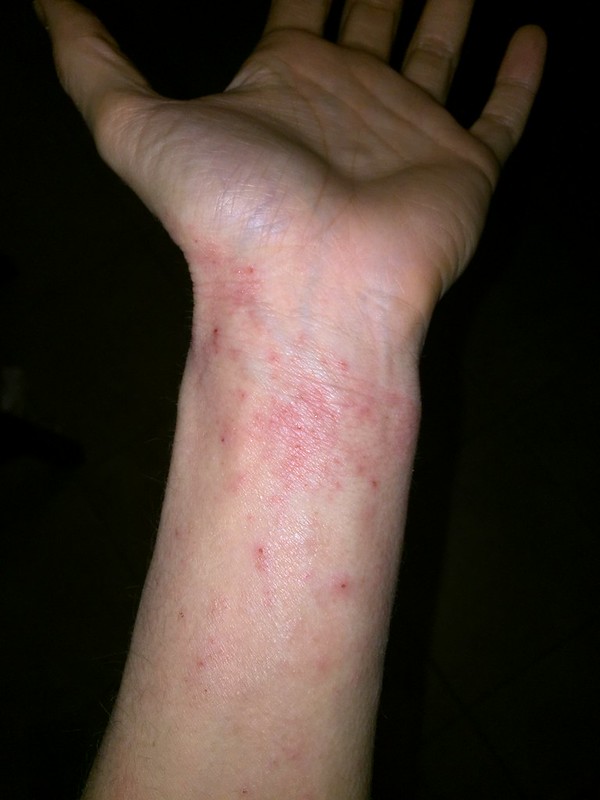
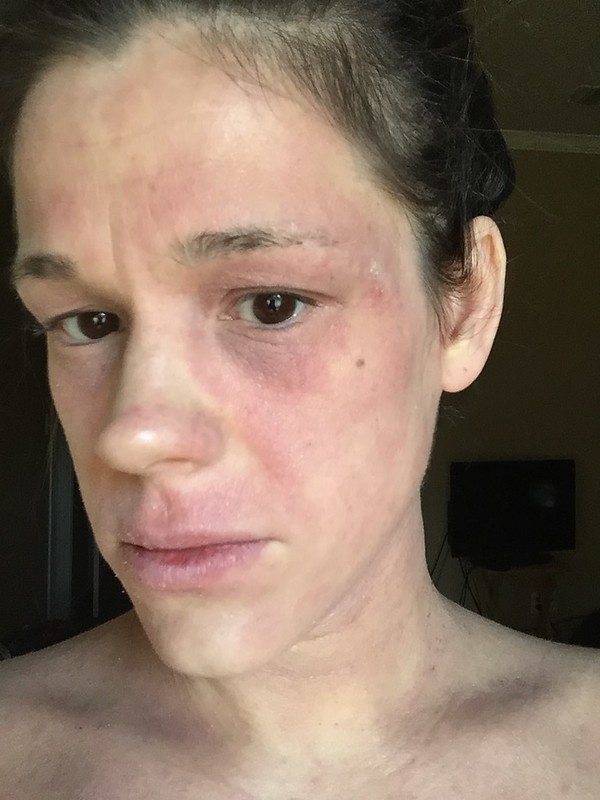
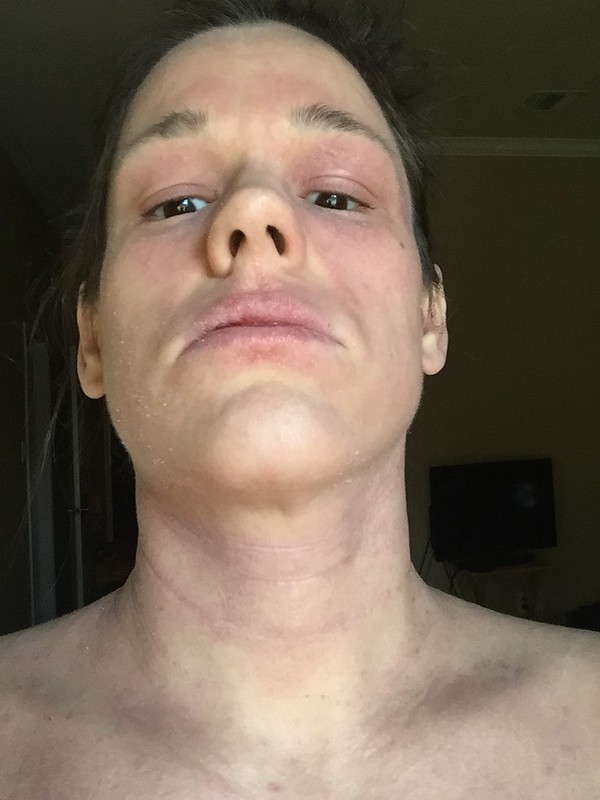
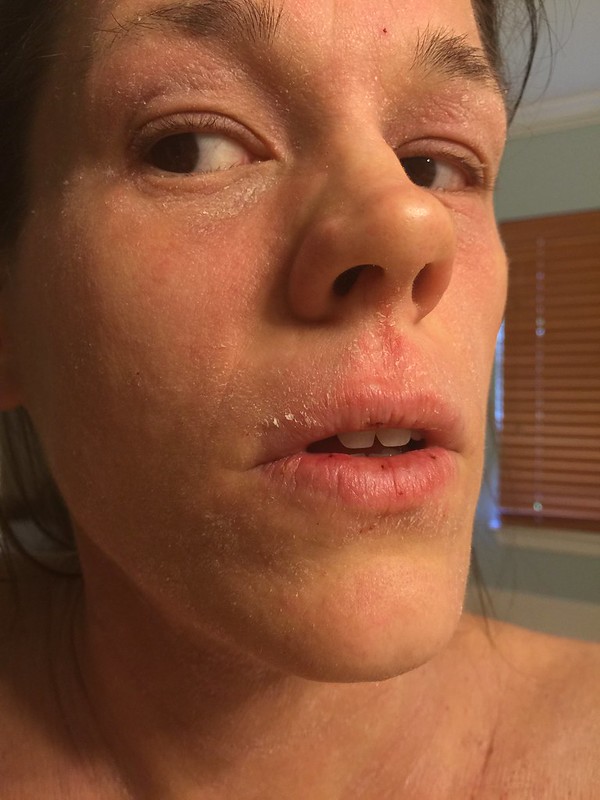
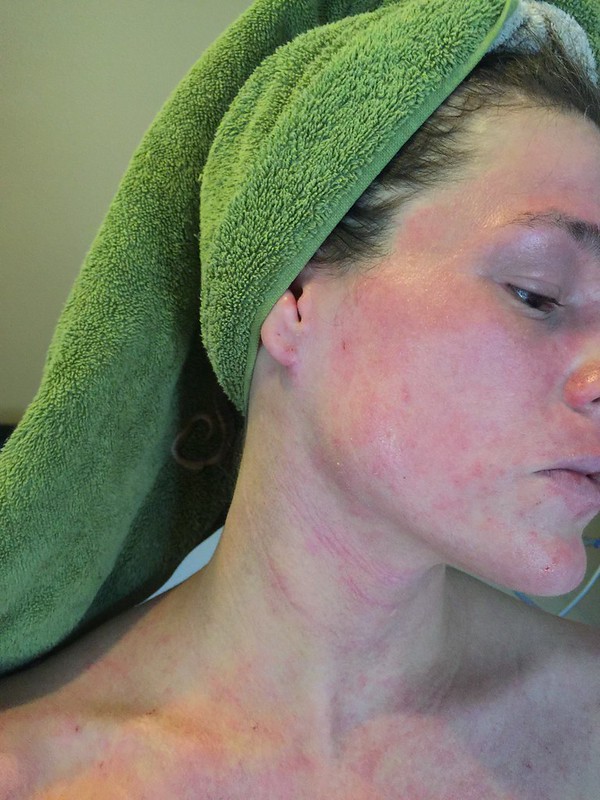
Regular fast food consumption raises the risk of asthma and eczema in children
They were also asked about their consumption of particular foods that were already associated with protective or damaging influences on health, including: fish meat veggies fruit bread pasta butter margarine rice pulses nuts milk eggs fast food/burgers Eating each of those foods was classified as never, occasionally, once or twice a week, or three or more times a week.
The experts controlled for variables that may have affected the results and found that the only type of food to have the same links across both age groups was fast food.
On analyzing their findings, the researchers proposed that “such consistency adds some weight to the possible causality of the relationship.”
Among all teens, consuming fast food was linked to current and severe symptoms of all 3 conditions, regardless of their gender, levels of affluence, or which country they were from.
Although the pattern among children was less convincing, there was still a link found between a fast food diet and symptoms except for current eczema, and poorer nations, except for present and severe asthma.
According to the authors, this dissimilarity may be due to the fact that kids have fewer choices when it comes to making food choices.
Three or more servings of fast food per week were associated with a 39% elevated risk of severe asthma among teens and a 27% increased chance among younger children, as well as to the severity of rhinitis and eczema, overall.
The experts discovered that fruit was protective in both age groups across all countries for all 3 conditions (current and severe) among kids, and among teens, for current and severe wheeze and rhinitis.
Consuming fruit 3 or more times per week was associated with a reduction in the severity of symptoms of 11% among teens and 14% among kids.
There are reasonable explanations for the results, the team pointed out. For example, high levels of saturated and trans fatty acids are found in fast food which can have an impact on immunity, while beneficial compounds and antioxidants are found in fruit.
The scientists stressed that this study did not demonstrate a cause and effect relationship, however, they said that more research is necessary.
The authors concluded:
“If the associations between fast foods and the symptom prevalence of asthma, rhinoconjunctivitis and eczema is causal, then the findings have major public health significance owing to the rising consumption of fast foods globally.”
Written by Sarah Glynn
Copyright: Medical News Today
Not to be reproduced without permission of Medical News Today
Visit our nutrition / diet section for the latest news on this subject. Do fast foods cause asthma, rhinoconjunctivitis and
eczema? Global findings from the International Study of Asthma and Allergies in Childhood (ISAAC) Phase Three
Philippa Ellwood, M Innes Asher, Luis Garcia-Marcos, Hywel Williams, Ulrich Keil, Colin Robertson, Gabriele Nagel, the ISAAC Phase III Study Group
THORAX 14 January 2013 doi:10.1136/thoraxjnl-2012-202285 Please use one of the following formats to cite this article in your essay, paper or report:
MLA
Glynn, Sarah. “Fast Food Linked To Asthma And
Eczema In Kids.” Medical News Today. MediLexicon, Intl., 15 Jan. 2013. Web.
7 Apr. 2013.
APA
Please note: If no author information is provided, the source is cited instead.
‘Fast Food Linked To Asthma And Eczema In Kids’
Please note that we publish your name, but we do not publish your email address. It is only used to let you know when your message is published. We do not use it for any other purpose. Please see our privacy policy for more information.
If you write about specific medications or operations, please do not name health care professionals by name.
All opinions are moderated before being included (to stop spam)
Contact Our News Editors
For any corrections of factual information, or to contact the editors please use our feedback form.

Please send any medical news or health news press releases to:
Note: Any medical information published on this website is not intended as a substitute for informed medical advice and you should not take any action before consulting with a health care professional. For more information, please read our terms and conditions.
View the original article here
Eczema Blog


























































/ABS/Auto%20Blog%20Samurai/data/Eczema%20Blog/e/256px-Fast_food_%2528282678968%2529.jpg)